A medical reversal is when an existing treatment is shown to be ineffective due to better quality research. Some estimates are than half of all medical treatments are ineffective or useless. And yet, despite the evidence that a treatment doesn’t work, many health-care providers continue to use them.
This is a call to action for these providers – if evidence doesn’t support a therapy then stop using it – even if you learned it in medical school. For patients, it’s an opportunity to realize that science and medical treatments are dynamic and evolve over time and your best source of understanding what works and what doesn’t work is not the internet – it’s a well-informed, critical thinking physician who is willing to abandon a treatment when evidence indicates it doesn’t work.
Medical care: A continuum from evidence to the mystical
Graduating from medical school doesn’t automatically mean you’re smart, or a critical thinker, just look at Dr. Oz.[1] [2] [3] But you don’t need to fill the coffers of Oz by watching his fantastical show to realize that physicians are people, and as such are susceptible to the emotional vagaries of our species. That’s the answer to why some physicians continue to offer treatments that that have been unambiguously shown to be ineffective, or, in some cases, deleterious to your health.
Case in point- the BRAT diet is an anachronism
I’ll offer a first-person example. A few months ago, I was concerned about a lingering gastroenteritis, so I scheduled an appointment to see my primary care physician. Unfortunately, she had no appointments available, so I ended up being seen by her nurse practitioner. As our conversation progressed, I found myself completely dismissing any further advice when I told her I was eating a normal diet and she responded that I should stop immediately and go on the BRAT (Bananas, Rice, Applesauce, Toast) diet.
I’m not a physician, but I read, and I knew that was truly an outdated recommendation that, by current standards, was consider not only ineffective, but in some cases had been shown to prolong symptoms. This is not a matter of opinion or perspective, there is ample literature and guidelines that clearly advise against the BRAT diet.[4] [5] [6] [7] And yet, there I was, sitting in a medical exam room with a nurse practioner giving me patently the wrong medical advice. But I’m sure in her mind it was simply a recommendation that has stood the test of time. I suppose one could call it a logical fallacy of argumentum ad antiquitatem (appeal to antiquity, appeal to tradition) [8], or maybe she simply had stopped learning after graduation and was unaware there was evidence that should have caused her to revise her approach to dietary recommendations for gastroenteritis.
The key word is evidence.
I don’t mean to unduly criticize medical practitioners – it’s a tough job. However, everyone must resist the urge to be an early adopter of an unproven treatment or cling to a treatment that has been reversed by new information. [9]
In medicine, a reversal can be defined as when a previously accepted and implemented practice has been shown to be ineffective by better quality or more powerful research. That’s quite different than a medical replacement which is when an existing treatment or practice that is effective is replaced because new evidence demonstrates a new treatment is a more effective.
That’s a distinction with a difference – a reversal curtails a treatment (or it should) because the treatment has been shown not to work. A replacement displaces a current, effective treatment with one that high-quality evidence has shown is more effective.
It’s a continuum
There is a continuum in healthcare that ranges from using the best evidence-based treatments to embracing the mystical treatments of alternative or complementary medicine. I can’t write that sentence without quoting a line from Tim Minchin’s short film – “You know what they call alternative medicine that’s been proved to work? – Medicine.” [10]
Because humans are an emotional species, we frequently make decisions, not by evaluating the evidence or facts, we “go with our gut” and then find facts to support that decision. The concept of motivated reasoning is a recurring theme running throughout this blog. [11] [12] [13] [14] [15] [16]
What’s the point?
What really precipitated this posting is a recent publication that caught my eye, “Meta-Research: A comprehensive review of randomized clinical trials in three medical journals reveals 396 medical reversals.”[17] Really? 396 reversals? This was news to me, but I soon realized that it was old news to many.
The subject of reversals and why physicians sometimes cling to the treatment that has been reversed has been a well-discussed topic for decades. Once again, I find myself in the familiar position of being in the dark on an important subject.
Let’s shed some light on it. Well, better yet, I’ll let Austin Frakt shed some light by quoting from his New York Times article, “Why Doctors Still Offer Treatments That May Not Help.” [18] Frakt begins by noting that when George Washington at age 67 became short of breath, [19] his attending physicians performed the treatment of the day and drained 40% of the blood from his body. [20] Whatever caused his shortness of breath probably wasn’t what killed him. Frakt continues by listing other instances of where medical treatments have been reversed:
There are countless other examples of common treatments and medical advice provided without good evidence: magnesium supplements [21] for leg cramps; oxygen therapy [22] for acute myocardial infarction; IV saline [23] for certain kidney disease patients; the avoidance of peanuts [24] to prevent allergies in children; many knee [25] and spine [26] operations; tight blood sugar control [27] in critically ill patients; clear liquid diets [28] before colonoscopies; bed rest [29] to prevent preterm birth; the prescribing [30] of unnecessary [31] medications, to list just a few. In some of these cases, there is even evidence of harm.
Below the waterline
As I discovered that’s just the tip of the iceberg. In 2013, 146 contradicted medical practices were reviewed in Mayo Clinic Proceedings [32] The reviewers concluded “Forty percent of the articles found the existing practice to be ineffective or harmful.” In the same year, Frakt posted an article where the title tells you everything you need to know, “Half of medical treatments of unknown effectiveness.” [33] In his article, Frakt provided the following chart from the source document in Clinical Evidence.
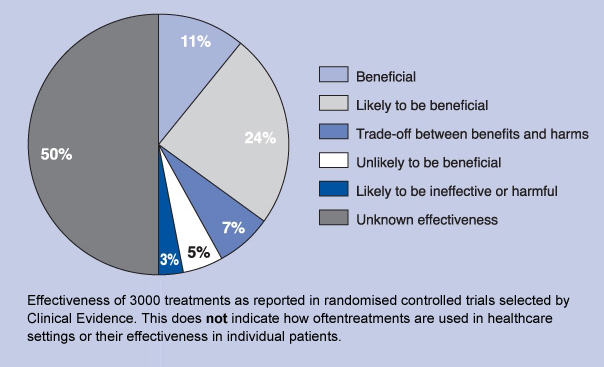
The discussions of medical reversals and why physicians are reticent to let go of unproven treatments are extensive. I’ll end this section with two quotes, the first is from a book review of “Ending Medical Reversal” [34] where the authors offered the following statement, “An old saw has long held that 50 percent of everything a student learns in medical school is wrong.” The data seems to support that percentage. The second quote may explain why that is. In “Hippocrates’ Shadow. Secrets from the House of Medicine,” [35] the author states “a logical theory often trumps reality.”
And, that brings us full circle back to the idea that humans tend to hold on to beliefs based on emotion rather than fact. It’s who we are. We know that offering unproven treatments is a bad idea, and yet we do. Something should change, we know it should, [36] but in the end, people will be people.
And the answer is…
Do you need to wait for high quality studies to establish the efficacy of every treatment? Are off label uses of medications acceptable? Is seeing a novel treatment work in one patient a sufficient reason to try it in another. Probably. Possibly. No.
This is where the experience of a physician come into play. He or she must balance evidence-based treatments against the temptation to push the envelope by considering new treatments with the bare minimum of date to receive FDA approval.
The dilemma often faced in medicine, as it is in life, is to not allow the perfect to be the enemy of the good.[37] That means some homework must be done by health-care workers. It’s not sufficient to listen to the polished, cherry-picked pitch from a pharmaceutical representative. It means actually reviewing the underlying studies that lead to FDA approval and determining if they are of high quality or if they lack the critical elements of medical research that cast doubt on their effectiveness and their role in patient care.
Every patient is an expert.
Physicians’ decisions about treatment strategies are informed not only by deciding when to abandon a treatment shown to be ineffective because of a medical reversal, but they are shaped by listening to the preferences of the patient. And thanks to the internet and the fact that the US is only one of two countries in the world (the other is New Zealand) that allows direct to consumer marketing (television commercials of prescription pharmaceuticals) [38], patients are increasingly coming to their appointments with internet-enabled self-diagnoses and a treatment they’ve seen on the television.
Medical reversals will continue to be a fact of life
As members of our emotion-guided species, both physicians and patients must be aware that many medical interventions will eventually be shown to be ineffective. We should all be comfortable with the reality that adopting a new treatment when a previous one has been shown not to work is not only a good intellectual idea – it’s good medicine.
Physicians can do their part by reading and understanding full journal articles (let’s talk about those p values and sample characteristics) and knowing when it’s time to let go of a treatment you may have learned in medical school and have been using for your patients for years.
Medical reversals and medical replacements are a fact of life that means the universe of treatments accepted as effective is dynamic and in a constant state of churn. But most important of all – never tell me again I should follow the BRAT diet! 😊
And for patients specifically, stop watching Dr. Oz, “researching” and diagnosing yourself on the internet, and believing you have the disease you’ve seen on the television and need the prescription medication being advertised to treat it.[39]
As is true with many decisions – the best ones are made when emotional influences are minimized, and logical assessments are maximized. Unfortunately, I think our species is a long way from that becoming our default decision-making approach.
[1] Real-world doctors fact-check Dr. Oz, and the results aren’t pretty. https://www.latimes.com/science/sciencenow/la-sci-sn-dr-oz-claims-fact-check-bmj-20141219-story.html
[2] Lies, fraud, conflicts of interest, and bogus science: The real Dr. Oz effect https://sciencebasedmedicine.org/lies-fraud-conflicts-of-interest-and-bogus-science-the-real-dr-oz-effect/
[3]Dr. Oz Makes Millions Even Though He’s Been Called A ‘Charlatan’ https://www.forbes.com/sites/michaelschein/2018/05/25/dr-oz-makes-millions-even-though-hes-a-total-fraud-and-other-reasons-you-should-follow-his-lead/#4f949a815fe1
[4] Practice Parameter: The Management of Acute Gastroenteritis in Young Children https://pediatrics.aappublications.org/content/pediatrics/97/3/424
[5] Managing Acute Gastroenteritis Among Children https://www.cdc.gov/mmwr/preview/mmwrhtml/rr5216a1.htm
[6] Acute Diarrhea in Adults https://www.aafp.org/afp/2014/0201/p180.html
[7] Diarrhea in Adults (Acute) https://www.aafp.org/afp/2008/0815/p503.html
[8] Appeal to Tradition (argumentum ad antiquitatem) https://www.logicallyfallacious.com/tools/lp/Bo/LogicalFallacies/44/Appeal-to-Tradition
[9] Persistence of Contradicted Claims in the Literature https://jamanetwork.com/journals/jama/fullarticle/209653
[10] Tim Minchin’s Storm the Animated Movie https://youtu.be/HhGuXCuDb1U?t=181
[11] Jindal’s berms: Critical thinking and politics https://confrontingmediocrity.net/2010/12/17/jindals_sand_berms/
[12] The Other National Deficit – Critical Thinking https://confrontingmediocrity.net/2013/06/16/the-other-national-deficit-critical-thinking/
[13] NPR endorses the magic of “Posture Guru” Esther Gokhale https://confrontingmediocrity.net/2015/08/12/npr-endorses-the-magic-of-posture-guru-esther-gokhale/
[14] We all lose when the news media reinforces the irrational fear of “stranger danger” https://confrontingmediocrity.net/2015/11/15/we-all-lose-when-the-news-media-reinforces-the-irrational-fear-of-stranger-danger/
[15] Belief-based thinking: Irrational fear of GMOs and Donald Trump as President. https://confrontingmediocrity.net/2017/02/20/belief-based-thinking-irrational-fear-of-gmos-and-donald-trump-as-president/
[16]Will logic and reason ever empower us to stop eating meat? https://confrontingmediocrity.net/2019/03/19/will-logic-and-reason-ever-empower-us-to-stop-eating-meat/
[17] Meta-Research: A comprehensive review of randomized clinical trials in three medical journals reveals 396 medical reversals https://elifesciences.org/articles/45183
[18] Why Doctors Still Offer Treatments That May Not Help https://www.nytimes.com/2019/08/26/upshot/why-doctors-still-offer-treatments-that-may-not-help.html
[19] Dec. 14, 1799: The excruciating final hours of President George Washington https://www.pbs.org/newshour/health/dec-14-1799-excruciating-final-hours-president-george-washington
[20] Death of a President https://www.nejm.org/doi/full/10.1056/NEJM199912093412413
[21] Effect of Magnesium Oxide Supplementation on Nocturnal Leg Cramps https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2603490
[22] Oxygen Therapy in Suspected Acute Myocardial Infarction https://www.nejm.org/doi/full/10.1056/NEJMoa1706222
[23] Trial Questions Hydration to Avoid Contrast-Induced Nephropathy https://www.medscape.com/viewarticle/876521
[24]Avoiding Peanuts to Avoid an Allergy Is a Bad Strategy for Most https://www.nytimes.com/2016/04/26/upshot/avoiding-peanuts-to-avoid-an-allergy-is-a-bad-strategy-for-most.html?module=inline
[25] Healthcare Triage News: Knee Surgery Doesn’t Improve Outcomes, but We Still Do A LOT of Them https://theincidentaleconomist.com/wordpress/healthcare-triage-news-knee-surgery-doesnt-improve-outcomes-but-we-still-do-a-lot-of-them/
[26] Spinal Fractures Can Be Terribly Painful. A Common Treatment Isn’t Helping. https://www.nytimes.com/2019/01/24/health/spinal-fracture-treatment.html?module=inline
[27] Glucose control in critical care https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4530321/
[28] Low-residue versus clear liquid diet before colonoscopy: a meta-analysis of randomized, controlled trials. https://www.ncbi.nlm.nih.gov/pubmed/26460222
[29] Lack of evidence for prescription of antepartum bed rest https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3226811/
[30] Habitual Prescribing of Laxatives—It’s Time to Flush Outdated Protocols Down the Drain https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2528287
[31]How Many Pills Are Too Many? https://www.nytimes.com/2017/04/10/upshot/how-many-pills-are-too-many.html?module=inline
[32] A Decade of Reversal: An Analysis of 146 Contradicted Medical Practices https://www.mayoclinicproceedings.org/article/S0025-6196(13)00405-9/abstract
[33] Half of medical treatments of unknown effectiveness https://theincidentaleconomist.com/wordpress/half-of-medical-treatments-of-unknown-effectiveness/
[34] Book Review: ‘Ending Medical Reversal’ Laments Flip-Flopping https://www.nytimes.com/2015/11/03/science/book-review-ending-medical-reversal-laments-flip-flopping.html?module=inline
[35] What Would Hippocrates Do?https://well.blogs.nytimes.com/2008/09/23/what-would-hippocrates-do/
[36] Medical Reversal: Why We Must Raise the Bar Before Adopting New Technologies https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3238324/
[37] This, and similar expressions, are often attributed to Voltaire who reference an Italian proverb “Il meglio è l’inimico del bene” (The best is the enemy of the good) in his Dictionnaire philosophique – puplished in 1770.
[38] Advertising drugs on the air waves? Yes, but only in the United States and New Zealand. https://confrontingmediocrity.net/2010/08/21/dtca/
[39] Big Pharma intensifies its efforts to tell you you’re sick. https://confrontingmediocrity.net/2017/03/19/big-pharma-intensifies-its-efforts-to-tell-you-youre-sick/
One thought on “How medical reversals impact your health care.”